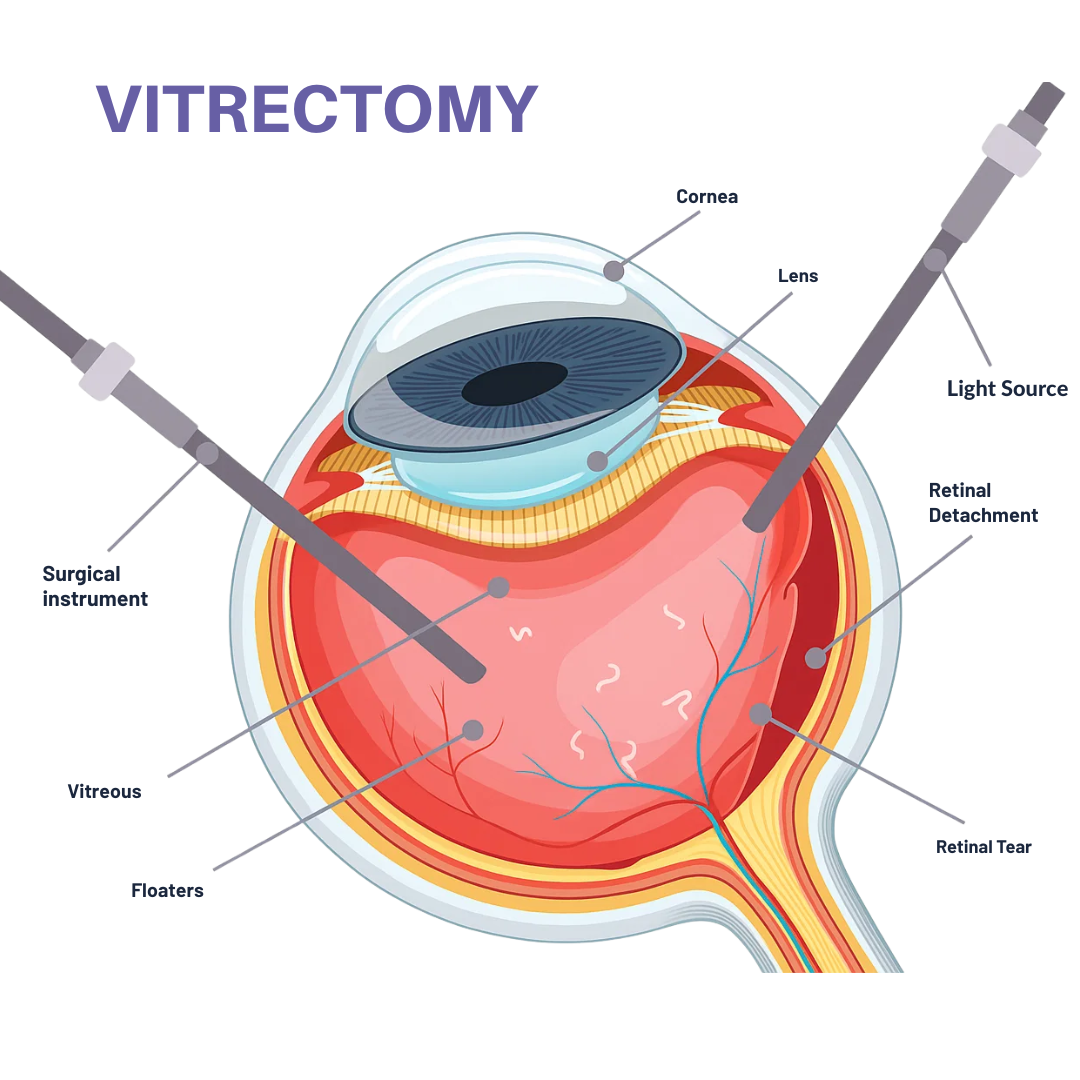
Understanding Vitrectomy Surgery
A vitrectomy is a specialized microsurgical procedure where an ophthalmologist removes the vitreous gel from the eye's interior. This delicate surgery treats various retinal conditions that can threaten your vision.
During the procedure, your surgeon uses precision instruments to remove clouded or problematic vitreous and repair underlying retinal damage. The surgery often involves injecting a gas bubble or silicone oil to support healing.
Success depends largely on proper post-surgical positioning and using appropriate recovery equipment during the healing process.
Conditions Treated with Vitrectomy
Macular Holes
Small tears in the macula that can cause central vision loss and distortion.
Retinal Detachment
Emergency condition where the retina separates from underlying tissue.
Diabetic Retinopathy
Diabetes-related damage to retinal blood vessels requiring surgical intervention.
Vitreous Hemorrhage
Bleeding into the vitreous cavity that obscures vision.
Epiretinal Membrane
Scar tissue formation on the retinal surface affecting central vision.
Severe Eye Trauma
Penetrating injuries requiring vitreous removal and retinal repair.
The Vitrectomy Procedure
Preparation & Anesthesia
The eye is numbed with local anesthesia. Three tiny incisions (less than 1mm) are made in the sclera.
Vitreous Removal
A specialized vitrectomy probe removes the clouded vitreous gel using controlled suction.
Retinal Repair
The surgeon addresses the underlying condition - repairing tears, removing scar tissue, or treating bleeding.
Gas or Oil Injection
A gas bubble or silicone oil may be injected to support retinal healing and maintain proper positioning.
Closure
The tiny incisions typically self-seal, and a protective patch may be applied over the eye.
Recovery Instructions
Detailed positioning instructions are provided, often requiring specialized recovery furniture.
Recovery Timeline & What to Expect
Week 1-2
- • Strict face-down positioning
- • Limited activities
- • Follow-up appointments
- • Eye protection essential
Week 3-4
- • Gradual positioning relaxation
- • Light activities resume
- • Gas bubble shrinking
- • Vision begins improving
Month 2-3
- • Vision stabilizing
- • Normal activities allowed
- • Gas bubble absorbed
- • Regular check-ups
Month 3-6
- • Full recovery achieved
- • Final vision assessment
- • All restrictions lifted
- • Success evaluation
Understanding Risks and Complications
Common Risks
- •Infection (rare, less than 1%)
- •Increased eye pressure
- •Cataract development
- •Retinal detachment recurrence
Learn more from the American Academy of Ophthalmology
Success Rates
Preparing for Your Vitrectomy
Before Surgery
- ✓Complete pre-operative testing
- ✓Arrange recovery equipment rental
- ✓Plan for assistance during recovery
- ✓Discuss medications with surgeon
Day of Surgery
- •Arrive 1-2 hours early
- •Bring insurance cards and ID
- •Wear comfortable, loose clothing
- •Follow fasting instructions
Post-Surgery Setup
- ⚡Recovery equipment delivered
- ⚡Positioning instructions reviewed
- ⚡Emergency contacts established
- ⚡Follow-up appointments scheduled
Expert Insights & Research
"The success of vitrectomy surgery depends not only on the surgical technique but critically on patient compliance with post-operative positioning requirements. Specialized recovery equipment significantly improves patient comfort and outcomes."
Recent Research Findings
A 2023 study published in the Journal of Retinal Surgery found that patients using specialized positioning equipment had 23% better compliance rates and improved surgical outcomes.
Clinical Guidelines
The Retina Society guidelines emphasize the importance of proper positioning equipment for optimal gas bubble mechanics and retinal adhesion.
Patient Education Resources
Internal Resources:
External Resources:
Finding the Right Vitrectomy Care
Choosing Your Surgeon
Finding an experienced retinal specialist is crucial for optimal outcomes. Look for surgeons with specific expertise in your condition and high success rates.
- • Board certification in ophthalmology
- • Fellowship training in vitreoretinal surgery
- • High volume of procedures performed
- • Access to latest surgical technology
Treatment Centers
Specialized retinal centers offer comprehensive care with advanced equipment, experienced teams, and coordinated support services for optimal patient outcomes.
- • Multi-disciplinary care teams
- • Advanced diagnostic equipment
- • Comprehensive support services
- • Emergency care availability
Understanding Your Specific Condition
Diabetic Retinopathy
Advanced diabetic eye disease requiring surgical intervention to prevent vision loss and manage complications from blood sugar damage.
Macular Conditions
Macular holes and epiretinal membranes affect central vision and require precise surgical repair for optimal visual outcomes.
Retinal Detachment
Emergency surgical condition requiring immediate intervention to restore retinal attachment and preserve vision.
Financial Planning & Insurance Coverage
Understanding Your Coverage
Vitrectomy surgery is typically covered by insurance when medically necessary. Understanding your benefits helps avoid unexpected costs and ensures proper authorization.
- • Pre-authorization requirements
- • In-network vs out-of-network benefits
- • Copayments and deductibles
- • Coverage for recovery equipment
Planning for Costs
Comprehensive financial planning includes surgical costs, recovery equipment rental, follow-up care, and potential time off work during healing.
Critical Recovery Phase: Why Positioning Matters
The success of your vitrectomy recovery depends critically on maintaining proper head positioning. When a gas bubble is used, it must remain in contact with the treated area of your retina.
Face-Down Positioning Requirements
- •Duration: Typically 1-2 weeks, sometimes up to 8 weeks depending on your condition
- •Compliance: 45-50 minutes per hour during waking hours
- •Sleep position: Face-down on stomach or side (as directed by surgeon)
- •Activities: Limited mobility; specialized equipment essential for comfort
⚠️ Critical Warning: Positioning Non-Compliance
Failure to maintain proper positioning can result in surgical failure, requiring repeat procedures. The gas bubble must stay in contact with your retina for optimal healing.
Equipment You'll Need
- • Face-down recovery chair
- • Adjustable recovery table
- • Positioning mirrors
- • Specialized pillows and cushions
- • Reading aids and entertainment
Recovery Timeline
Make Your Recovery Comfortable & Successful
Our specialized vitrectomy recovery equipment ensures proper positioning while maintaining your comfort and dignity during the critical healing period.
Free delivery • Expert setup • 24/7 support during your recovery
